Cleanings & Gum Disease Treatment in South Fort Worth
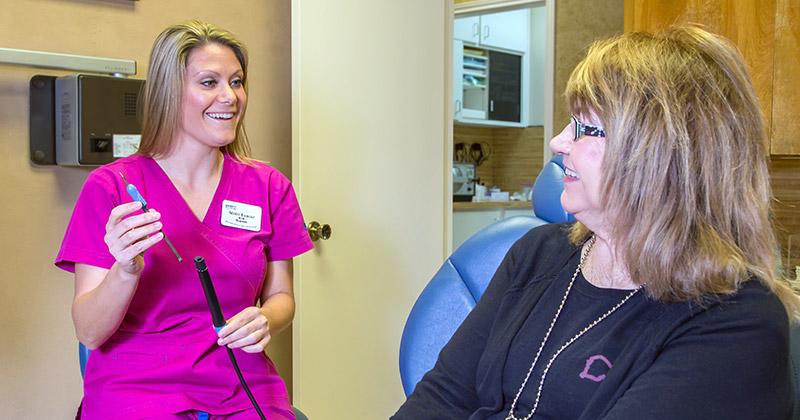
Our friendly hygienists are highly experienced and will provide you with comfortable yet thorough cleanings.
Keeping Your Teeth Healthy for Life!
- Gentle, Effective Gum Disease Treatment
- What Is Scaling and Root Planing?
- Ultrasonic Scalers for Maximum Comfort
- $89 New Patient Special
Regular teeth cleanings and proper at-home care are two of the best guarantees for strong, healthy teeth that will last you a lifetime. Dr. Warren and his staff use modern tools and techniques to keep your teeth sparkling and your gums healthy. Regular cleanings help identify potential problems and allow us to treat them before they get worse.
Comfortable, Thorough Dental Cleanings
Our friendly, competent hygienists are highly experienced when it comes to patient care and comfortable, thorough teeth cleanings. They use advanced equipment to achieve great results, including the Prophy Jet, an air-polishing device for heavy plaque and stain removal. The Prophy Jet combines air, water and baking soda to gently blast away bacteria and debris, leaving teeth sparkling and squeaky clean.
Education on home oral care

Your hygienist will educate you on how to best take care of your teeth at home between visits.
Proper at-home care is vital for keeping teeth and gums healthy and functioning. For that reason, our friendly, caring hygienists will take the time to educate you on best oral hygiene practices. They will use a combination of teaching aids—displays, literature and models—to show you the proper techniques and coach you into being able to perform them well. We like to think of ourselves as your partners in the maintenance of your oral health.
Gentle, Effective Gum Disease Treatment
Gum disease is the #1 reason for adult tooth loss in the United States, but unfortunately, it is often a symptomless disease, going untreated while causing unsuspected damage to the gums, teeth and bone. Untreated gum disease has many harmful effects on your oral and overall health and can result in tooth loss. Early detection of gum disease is vital to preventing the damage it can cause.
We are able to take care of any gum disease, whether mild or severe, and help you get it under control.
Scaling and root planing
Scaling is a nonsurgical, careful cleaning of your teeth to remove the accumulated hardened plaque and bacteria, called calculus. Calculus deposits cause inflammation of the surrounding gum. This causes the gum to pull away from your teeth, creating deep pockets where bacteria can thrive.
Root planing is done to smooth out the surface of your tooth roots, making it difficult for new bacteria to lodge there.
Scaling and root planing are together known as “deep cleaning” and are an effective means of treating gum disease.
Ultrasonic scalers for maximum comfort and effectiveness
 We use ultrasonic scalers as part of your scaling and root planing procedure. They are efficient and effective for removing plaque and heavy stains. By means of high-speed vibrations, ultrasonic scalers chip away tough, hardened plaque called “calculus.” At the same time, a cooling stream of water keeps the scaler from generating heat while also washing away the dislodged calculus.
We use ultrasonic scalers as part of your scaling and root planing procedure. They are efficient and effective for removing plaque and heavy stains. By means of high-speed vibrations, ultrasonic scalers chip away tough, hardened plaque called “calculus.” At the same time, a cooling stream of water keeps the scaler from generating heat while also washing away the dislodged calculus.
The ultrasonic vibrations generated by our scalers also produce a shockwave which destroys the cell membranes of the bacteria in plaque, effectively killing them.
Ultrasonic scalers are gentler on your teeth than traditional hand instruments.
$89 New Patient Special—Exam, X-rays & Consultation
Take advantage of our New Patient Special and receive a comprehensive oral exam, X-rays and consultation. Your visit will include:
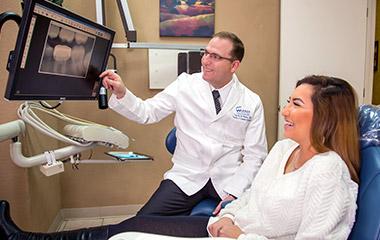
- Exam
- Full set of X-rays
- Panoramic X-rays
- Oral cancer screening
- Consultation with the doctor
- Treatment options
- Get your questions answered
To make an appointment, call 817‑241‑2820 or click here to request an appointment online.
